Introduction
n the intricate world of healthcare technology, the role of a software architect is not just pivotal but also fraught with unique challenges that vary from country to country. Alex (not his real name), a visionary software architect, led a high-stakes healthcare project in a government organization. This blog post explores how he navigated not just the complexities of healthcare interoperability but also the stringent deployment constraints that differ across countries. From data storage laws in France to tool enforcement protocols, discover how Alex successfully built a future-proof, compliant, and scalable healthcare system.
Problem Statement: The Challenge of Interoperability
Interoperability in healthcare is more than just a buzzword; it’s a critical requirement. The healthcare sector involves a myriad of stakeholders—from pharmacies and insurance companies to healthcare providers —creating a system that communicates seamlessly is no small feat. The challenge is further amplified by the sensitive nature of healthcare data, which demanded high levels of security and compliance.
Alex’s project was under the spotlight for several reasons. First, working through a solution vendor, the client was part of a government initiative, which meant it was subject to intense scrutiny and regulatory oversight. Second, the project had a tight deadline due to an upcoming healthcare reform, leaving little room for error or delays. Lastly, budget constraints added another layer of complexity, limiting the resources available for tackling this multifaceted problem.
The stakes were high, and the margin for error was low. Alex, with his visionary traits, saw this as an opportunity rather than a hindrance. He believed that constraints often lead to innovation, and he proved it.
Components at Play: The Intricate Web of Systems and Stakeholders
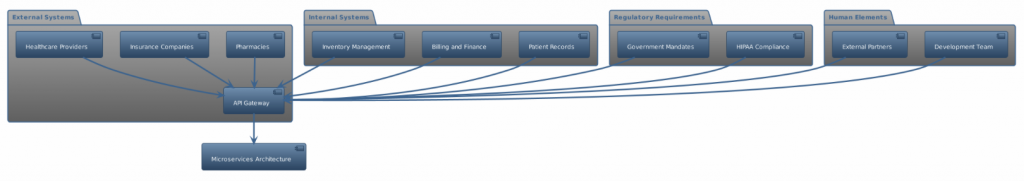
In any healthcare project, the ecosystem is vast and interconnected. Alex had to consider various components, each with its own set of requirements, limitations, and challenges. Here are some of the key components that were at play:
External Systems
- Pharmacies: Required real-time access to prescription data.
- Insurance Companies: Needed to validate coverage and process claims.
- Healthcare Providers: Particularly across clinicians, required seamless data sharing for patient history, treatments, and medications.
Internal Systems
- Patient Records: A centralized database that had to be both secure and easily accessible.
- Billing and Finance: Systems that needed to integrate with both internal patient records and external insurance companies.
- Inventory Management: For tracking medical supplies and medications.
Regulatory Requirements
- HIPAA Compliance: Ensuring the privacy and security of sensitive healthcare data.
- Government Mandates: Adhering to healthcare reform policies and other legal requirements.
Human Elements
- Development Team: A mix of junior and experienced developers.
- External Partners: Teams from pharmacies, insurance companies, and healthcare providers who had their own systems and protocols.
Balancing Innovation and Practicality
Alex knew that the key to solving the interoperability challenge lay in creating a robust architecture that could serve both current and future needs. His visionary approach was to design a microservices architecture that allowed for modularity and scalability.
He started by organizing a series of workshops with both internal and external stakeholders. These workshops aimed to identify the pain points in the existing systems and to brainstorm potential solutions. Alex’s excellent communication skills were crucial here; he was able to articulate his long-term vision while also addressing immediate concerns.
One of the innovative solutions Alex proposed was the use of an API gateway. This would act as a mediator between different systems, translating various API protocols into a language that each system could understand. It was a simple yet effective solution that addressed the primary challenge of interoperability while also laying the groundwork for future scalability.
Overcoming Challenges: The Path to Resolution
The clock was ticking, and the pressure was mounting. Despite the constraints, Alex remained steadfast in his commitment to innovation. He knew that the key to overcoming the challenges lay in meticulous planning and effective execution.
Tight Deadlines
Alex tackled the issue of tight deadlines by adopting an Agile methodology, allowing the team to work in sprints and prioritize tasks effectively. This approach provided the flexibility to adapt to changes quickly and ensured that the most critical components were developed first.
Limited Budget
To address the budget constraints, Alex focused on utilizing open-source technologies wherever possible, reducing the overall cost. He also advocated for investing in automated testing and continuous integration tools to speed up the development process and reduce long-term maintenance costs.
Mixed Team Expertise
Alex leveraged the strengths of his mixed-experience team by assigning tasks based on individual expertise. Junior developers were paired with more experienced team members for mentorship, while the seasoned developers tackled the more complex aspects of the architecture.
High Data Sensitivity
Given the sensitive nature of healthcare data, Alex prioritized security from the get-go. He implemented robust encryption methods and ensured that all data transmissions were secure. Regular security audits were conducted to identify and fix any vulnerabilities.
The Resolution: A Future-Proof Healthcare System
After months of hard work, the team, under Alex’s visionary leadership, successfully launched the new healthcare management system. The API gateway was a resounding success, effectively solving the interoperability issue. The system was not only compliant with all regulatory requirements but also scalable, setting the stage for future expansions and improvements.
Alex’s ability to balance his visionary ideas with practical solutions proved to be the linchpin of the project’s success. He demonstrated that even under tight constraints, innovation is not only possible but can also lead to robust, future-proof solutions.
Deployment Constraints Across Different Countries in Healthcare
Data Storage
- Data Sovereignty: In countries like France, healthcare data must be stored within the country’s borders to comply with data sovereignty laws. This can be a significant constraint for cloud-based solutions that use data centers located in other countries.
- Data Encryption: Strict regulations often require that healthcare data be encrypted both in transit and at rest. The encryption algorithms and key management practices may also be subject to local laws.
- Backup and Recovery: Countries may have specific requirements for data backup and recovery, including the frequency of backups and the duration for which backups must be retained.
Tool Enforcement
- Certification of Tools: Some countries require that software tools used in healthcare be certified by a governmental or accredited body. For example, in France, healthcare software must often be certified by the Haute Autorité de Santé (HAS).
- Interoperability Standards: Countries may enforce specific standards for healthcare data exchange, such as HL7 or FHIR, which can limit the tools that can be used.
- Audit Trails: Tools must often provide comprehensive audit trails that record who accessed what data, when, and what actions they took. This is crucial for compliance with privacy laws.
Version Control
- Regulatory Approval: Any changes to the software, including updates and patches, may need to be approved by regulatory bodies. This can slow down the deployment of new versions.
- Documentation: Extensive documentation is often required for each version of the software, detailing what changes have been made, how they were tested, and how they affect compliance with local laws.
- Legacy Systems: Older versions of software may still be in use due to long approval cycles for new versions, leading to compatibility issues.
Conclusion
Alex’s journey in leading this complex, multi-country healthcare project serves as an inspiring case study for software architects and project managers alike. His visionary approach, coupled with an in-depth understanding of international deployment constraints, turned challenges into opportunities for innovation. The project not only met its immediate goals but also laid a strong foundation for future healthcare reforms and international deployments. Alex’s story is a testament to the power of visionary leadership and meticulous planning in overcoming not just technical but also regulatory hurdles in healthcare technology.
FAQs with Answers
Q: What is healthcare interoperability?
A: Healthcare interoperability refers to the ability of different healthcare systems to work together and share information as seamlessly as possible. It’s crucial for improving patient care, reducing costs, and enhancing the efficiency of healthcare services.
Q: What role does a software architect play in healthcare projects?
A: A software architect is responsible for designing the system and software architecture, making technology choices, and ensuring that the project meets its functional and non-functional requirements. They also play a key role in stakeholder management and problem-solving.
Q: Why is a microservices architecture beneficial for healthcare systems?
A: Microservices architecture allows for greater modularity and scalability. It enables different components of the healthcare system to operate independently, making it easier to update, scale, and maintain the system.
Q: How can API gateways solve interoperability issues?
A: An API gateway acts as a mediator between different systems, translating various API protocols into a language that each system can understand. This simplifies the process of integrating multiple systems and enhances interoperability.
Q: What are the challenges of working on a government healthcare project?
A: Government healthcare projects often come with tight deadlines, budget constraints, and high levels of regulatory oversight. They also involve multiple stakeholders, both internal and external, adding layers of complexity to the project. From an software architecture and engineering operational perspective, the layers can go deep, especially if the organization is going to be installed across multiple countries, such as where data is stored or what version control systems to use.


2 thoughts on “Software Architect’s Resolve in a Complex Healthcare Project”